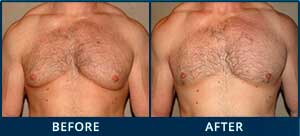
Nipple Repositioning and Skin Excision: When is it necessary?
As a plastic surgeon specializing in gynecomastia surgery, I come across chests of all shapes and sizes. Gynecomastia can present in a variety of ways, from small glandular firmness under the nipple to full-on breasts with ptosis, or droopiness. For most gynecomastia cases, removal of the excess tissue, whether it is with excision, liposuction, or both, is enough to get the ideal contour. This is because the skin tends to tighten and re-drape over the deeper muscles.
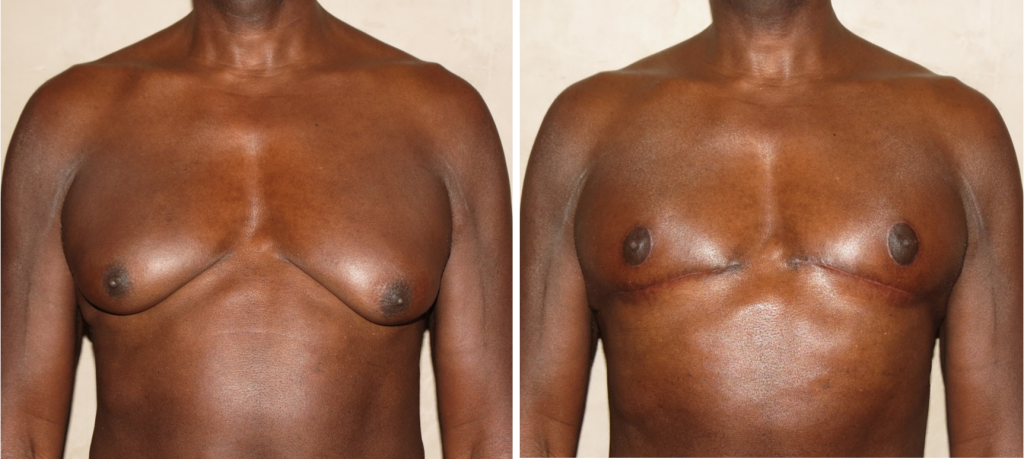
However, in certain cases just removing the excess tissue is not enough to obtain the ideal contour. This is the case in males who not only have excess tissue, but also excess skin and nipples that are too low on their chests. In these patients, if the nipple position and skin excess are not addressed, simply taking out the excess tissue will likely leave them with a deflated and looking breast with sagging skin and nipples.
In these specific cases it is necessary to reposition the nipples to a normal location as well as remove the excess skin. This can be done by leaving the nipple on a base of breast tissue while removing the rest of the tissue around it and removing the excess skin. Another option is to remove the nipple and areola, excise all of the excess tissue and skin, then place the nipple and areola as a free graft in the appropriate position. The advantage of the first technique is that it may have a higher chance of maintaining nipple sensation and projection, but the disadvantage is that there will still be some fullness under the areola because of the tissue that needs to be left behind to provide blood supply to the nipple. The advantage of the free graft technique is that it will give the flattest contour with the disadvantage being numbness of the nipple, possible loss of nipple projection, and possible areolar depigmentation.
However, when the gynecomastia is severe with loose skin and low nipples, this is the best technique to perform. I always advise these patients that they need to be okay with the incisions necessary to obtain the results they are after. If they are not willing to accept the incisions, then they should not have gynecomastia surgery.
To learn more about gynecomastia surgery and to see before and after photographs, visit www.losangelesgynecomastia.org.
Mondor’s Thrombophlebitis
From time to time, patients who undergo gynecomastia surgery come in for their 1 month follow up and say that they feel a firm, rope-like structure on their abdomen or chest. They usually say they noticed it around 2-4 weeks after surgery. Sometimes it is painful, sometimes not. Obviously they are very concerned especially because in some cases it occurs in an area which did not even undergo surgery.
The most important thing I can do is to reassure them. What they are referring to is Mondor’s cords or thrombophlebitis. This is an inflammation of the superficial veins that run under the skin in the upper abdomen and chest. They can become inflamed which leads to that hard rope- like feel. Mondor’s cords typically resolve on their own, although sometimes anti-inflammatories can be helpful with symptoms of pain. Below is an example of a patient of mine who underwent gynecomastia surgery without any procedures on his abdomen. One can see the Mondor’s cords on the image on the left at 4 weeks post-surgery. At his 3 month visit they are completely gone.
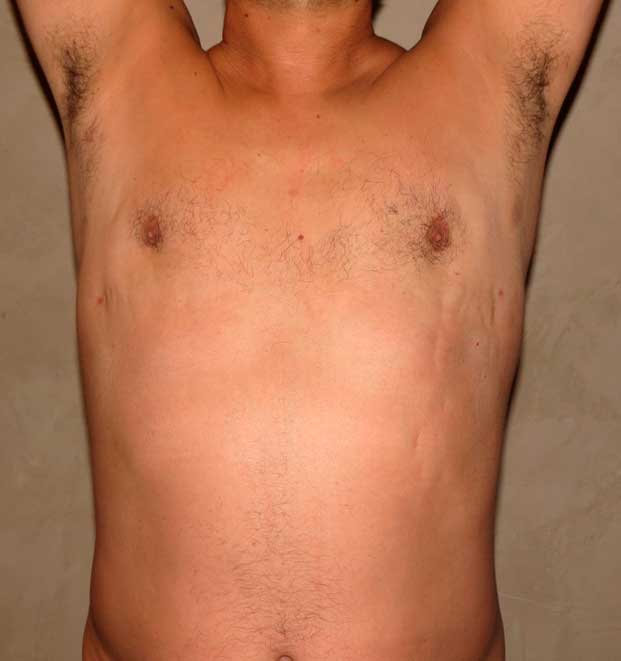
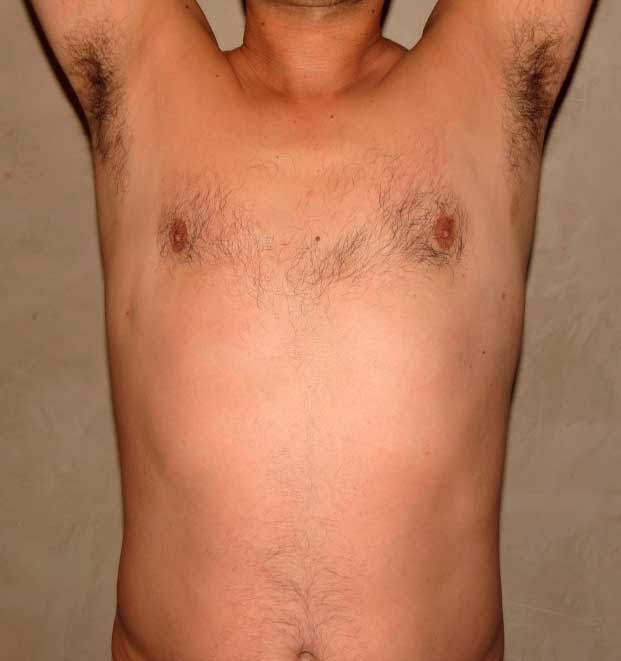
To learn more about gynecomastia surgery and to see before and after photographs, visit www.losangelesgynecomastia.org.

 Español
Español Português
Português Italiano
Italiano 日本語
日本語 Deutsch
Deutsch Français
Français 中文
中文 العربية
العربية Русский
Русский עִברִית
עִברִית